Introduction
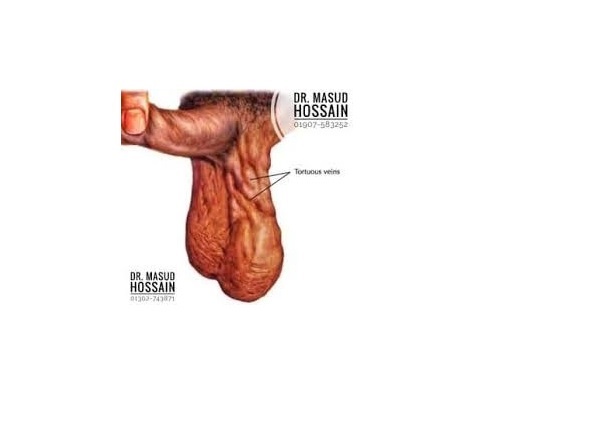
Testicular prolapse, also known as testicular torsion or testicular hernia, is a medical condition where one or both testicles descend from the scrotum into the groin or abdomen. This condition can cause severe discomfort and pain and requires prompt medical attention. This article explores the causes, symptoms, and available treatment options for testicular prolapse while emphasizing the importance of seeking immediate medical help when experiencing such symptoms.
Understanding Testicular Prolapse
Testicular prolapse occurs when the spermatic cord, which supplies blood to the testicles, becomes twisted, cutting off blood flow to the testicle(s). This medical emergency requires swift intervention to prevent potential complications, such as testicular damage or infertility.
Causes of Testicular Prolapse
Several factors can contribute to testicular prolapse, including:
- Physical Trauma: Injury or trauma to the groin area can lead to testicular prolapse.
- Strenuous Activities: Engaging in vigorous physical activities or sports without adequate support or protection can increase the risk.
- Congenital Factors: Some individuals may have a predisposition to testicular torsion due to the way the testicle is attached inside the scrotum.
- Cold Weather: Exposure to cold temperatures can cause the scrotum to contract, potentially leading to torsion.
Symptoms of Testicular Prolapse
Recognizing the signs of testicular prolapse is crucial for timely intervention. Common symptoms include:
- Sudden and Severe Testicular Pain: Sharp and intense pain in the testicles, often accompanied by swelling.
- Abdominal Pain: Some individuals may experience abdominal pain, nausea, or vomiting.
- Frequent Urination: Painful or increased frequency of urination can be a symptom of testicular torsion.
- Changes in Testicle Position: The testicle may appear higher in the scrotum or completely out of place.
Treatment Options
- Emergency Medical Care: Testicular prolapse is a medical emergency. If symptoms occur, it is essential to seek immediate medical attention. Doctors will conduct a physical examination and may use ultrasound to confirm the diagnosis.
- Manual Detorsion: In some cases, a doctor can manually untwist the spermatic cord, restoring blood flow to the testicle. This procedure must be done promptly and by a medical professional.
- Surgery: Surgery is often necessary to prevent recurrence. During surgery, the testicle is surgically attached to the inner lining of the scrotum to prevent future torsion episodes.
- Orchiopexy: Orchiopexy is a surgical procedure where the testicle is permanently attached to the scrotum, reducing the risk of torsion.
Prevention and Self-Care
While some cases of testicular prolapse cannot be prevented, there are steps individuals can take to reduce the risk:
- Wear Protective Gear: Athletes should wear protective cups during sports activities to reduce the risk of injury.
- Avoid Trauma: Be cautious and aware of the surroundings to avoid accidental injuries to the groin area.
- Regular Self-Examination: Regularly checking the testicles for any changes in size, shape, or tenderness can help detect potential issues early.
Conclusion
Testicular prolapse is a serious medical condition that demands immediate attention. Recognizing the symptoms and seeking prompt medical care are crucial to preserving testicular health and preventing complications. It is essential for individuals to be aware of the risk factors and take preventive measures, such as wearing protective gear during sports, to minimize the chances of testicular injury. By staying informed and proactive, individuals can contribute to the early detection and effective management of testicular prolapse, ensuring the best possible outcome and quality of life.